When we think about our overall health, we often consider factors like diet, exercise, and lifestyle choices. However, there's an essential aspect of well-being that sometimes goes overlooked—our eye health.
Your eyes can offer valuable insights into your overall health, especially when it comes to chronic conditions like diabetes and hypertension. In this blog post, we'll explore the intricate relationship between these conditions and eye health, focusing on diabetic retinopathy and hypertensive retinopathy.
The Eyes as Windows to Health
Your eyes are not only the windows to your soul, but they can also be windows to your health. The blood vessels in your eyes are tiny and delicate, making them sensitive to changes in your overall circulatory health. Conditions like diabetes and hypertension can have a profound impact on these delicate vessels.
Diabetes and Diabetic Retinopathy
Diabetes, a chronic condition characterized by high blood sugar levels, is a significant risk factor for eye problems. One of the most common eye complications associated with diabetes is diabetic retinopathy.
It occurs when high blood sugar levels damage the blood vessels in the retina, the light-sensitive tissue at the back of the eye responsible for transmitting visual signals to the brain. Diabetic retinopathy often progresses silently, without noticeable symptoms in the early stages, making regular eye exams crucial for early detection and treatment.
How Does Diabetic Retinopathy Develop?
The development of diabetic retinopathy typically follows these stages:
- Background Retinopathy: In the early stage, small blood vessels in the retina weaken and may leak tiny amounts of blood or fluid, causing no immediate symptoms.
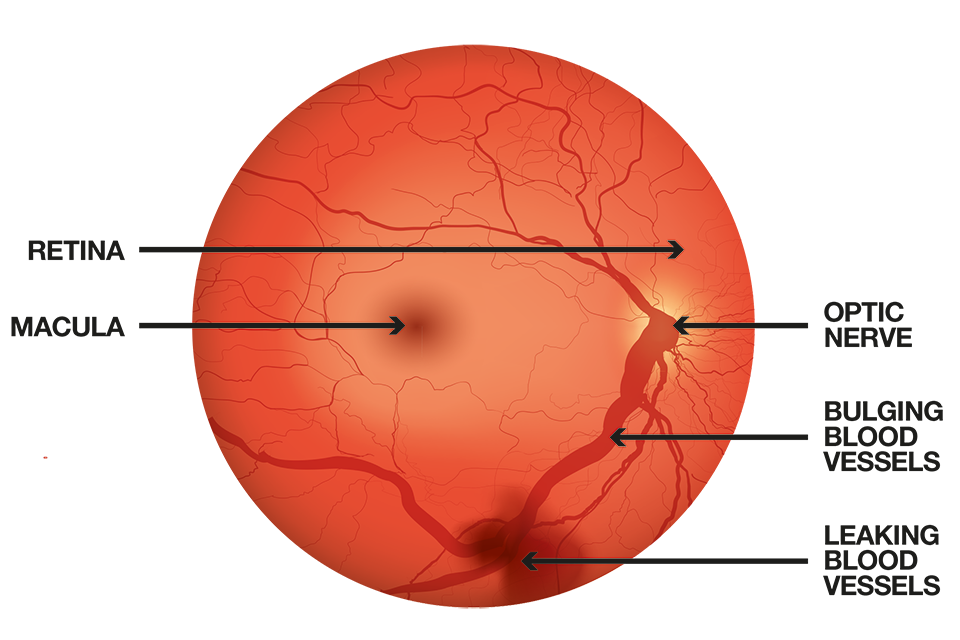
- Macular Edema: When fluid accumulates in the macula (the central part of the retina responsible for sharp, central vision), it can lead to blurred vision and distortion.
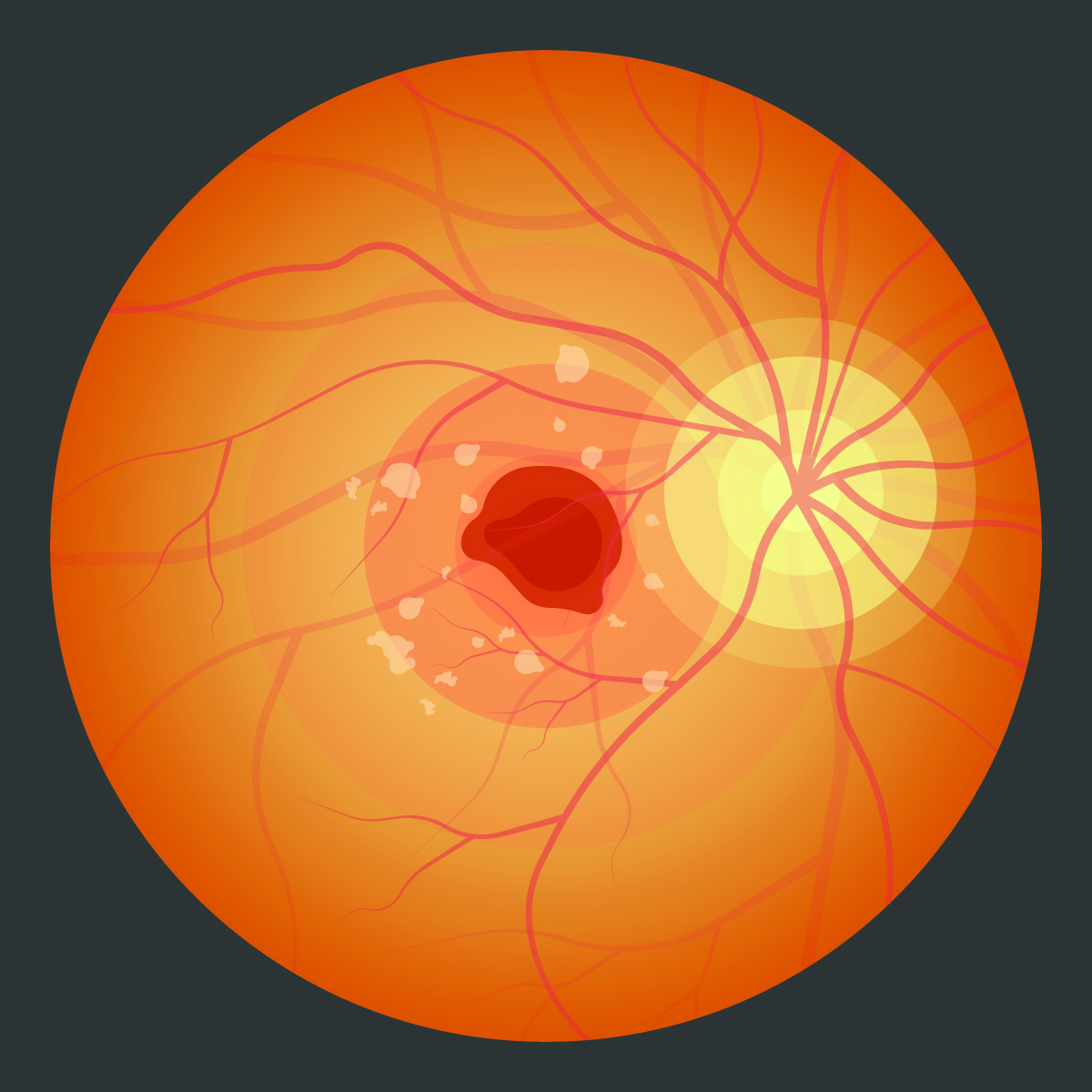
- Proliferative Retinopathy: In the advanced stage, the retina starts growing new blood vessels, which are fragile and prone to bleeding. This stage can lead to severe vision loss and even blindness.

Common Symptoms and Risk Factors
While diabetic retinopathy may not show symptoms in its early stages, as it progresses, individuals may experience:
- Blurred or fluctuating vision

- Floaters (dark spots or strings in vision)

- Difficulty seeing in low light conditions

- Loss of peripheral vision

Several factors increase the risk of developing diabetic retinopathy:
- Poorly controlled blood sugar levels
- High blood pressure
- Duration of diabetes
- High cholesterol levels
- Smoking
- Pregnancy (gestational diabetes)
Preventing and Managing Diabetic Retinopathy
- Regular Eye Exams: Early detection and timely treatment are crucial. People with diabetes should have a comprehensive eye examination at least once a year, or as recommended by their eye care specialist.

- Blood Sugar Control: Maintaining good blood sugar control through a healthy diet, regular exercise, and prescribed medications or insulin can significantly reduce the risk of diabetic retinopathy.
- Blood Pressure Management: Managing high blood pressure and cholesterol levels can help protect your eyes and overall health.

- Lifestyle Choices: Quitting smoking and adopting a healthy lifestyle can have a positive impact on your eye health.

- Treatment Options: If diabetic retinopathy is detected, treatment options may include laser therapy, injections, or surgery, depending on the severity of the condition.
Hypertension and Hypertensive Retinopathy
Hypertension, or high blood pressure, is another chronic condition that can affect eye health. When blood pressure remains consistently elevated, it can lead to a condition known as hypertensive retinopathy.

How Does Hypertensive Retinopathy Develop?
-
Stage 1: Mild Hypertensive Retinopathy - Early signs include narrowing of the blood vessels, increased curvature, and copper or silver wire appearance of the arteries. These changes are usually asymptomatic.
-
Stage 2: Moderate Hypertensive Retinopathy - As blood pressure continues to rise, more noticeable changes occur, including hemorrhages, cotton-wool spots (nerve fiber layer infarcts), and exudates (lipid or protein deposits).
-
Stage 3: Severe Hypertensive Retinopathy - In advanced stages, the retina may experience swelling (edema), macular star formation (exudates radiating from the macula), and optic nerve head swelling.
-
Stage 4: Malignant Hypertensive Retinopathy - This is the most severe form, characterized by widespread retinal damage, retinal detachment, and optic nerve damage. It can lead to permanent vision loss if not treated urgently.
Common Symptoms and Risk Factors
In its early stages, hypertensive retinopathy may not manifest noticeable symptoms. However, as the condition progresses, individuals may experience:
- Blurred vision

- Headaches

- Visual disturbances, such as seeing spots or floaters

- Vision loss

Several factors increase the risk of developing hypertensive retinopathy:
- Uncontrolled high blood pressure
- Long-standing hypertension
- Smoking
- Diabetes
- Kidney disease
- Obesity
- High cholesterol levels
Preventing and Managing Hypertensive Retinopathy
-
Blood Pressure Control: Maintaining healthy blood pressure levels through medication, lifestyle changes, and regular monitoring is the most critical step in preventing and managing hypertensive retinopathy.
-
Regular Eye Exams: Routine eye examinations can detect early signs of hypertensive retinopathy, allowing for timely intervention and treatment.
-
Medication and Lifestyle Modifications: Consult with a healthcare professional to develop a comprehensive plan for managing hypertension. This may include prescribed medications, dietary changes, exercise, and stress reduction techniques.
-
Quit Smoking: Smoking can exacerbate hypertension and increase the risk of eye and cardiovascular problems. Quitting smoking is essential for overall health.
-
Early Treatment: If hypertensive retinopathy is diagnosed, treatment may include blood pressure management and, in advanced cases, laser therapy or surgery to prevent further vision loss.
In conclusion, it's essential to recognize that our eyes are not just the windows to our souls but also valuable indicators of our overall health. Diabetes and hypertension, two prevalent chronic conditions, can have a profound impact on our eye health, leading to diabetic retinopathy and hypertensive retinopathy, respectively.
Both diabetic retinopathy and hypertensive retinopathy can progress silently, often without noticeable symptoms in their early stages. This underscores the critical importance of regular eye examinations, which can detect these conditions at an early, treatable stage.
For those living with diabetes, maintaining optimal blood sugar control, managing blood pressure and cholesterol levels, adopting a healthy lifestyle, and attending routine eye exams are essential steps in preventing and managing diabetic retinopathy.
Similarly, for individuals dealing with hypertension, controlling blood pressure through medication, lifestyle modifications, and regular monitoring is crucial. Regular eye examinations can detect hypertensive retinopathy early, enabling timely intervention to prevent vision loss.
Incorporating these measures into your healthcare routine not only safeguards your vision but also promotes your overall well-being. Remember, prioritizing your eye health goes hand in hand with maintaining a healthy lifestyle and effectively managing chronic conditions like diabetes and hypertension. By taking proactive steps, you can enjoy a lifetime of clear vision and better health.

